Guarding Against Metabolic Diseases
Through Research Based Preventive Treatments
61% of Indonesians are Affected by Hypertension
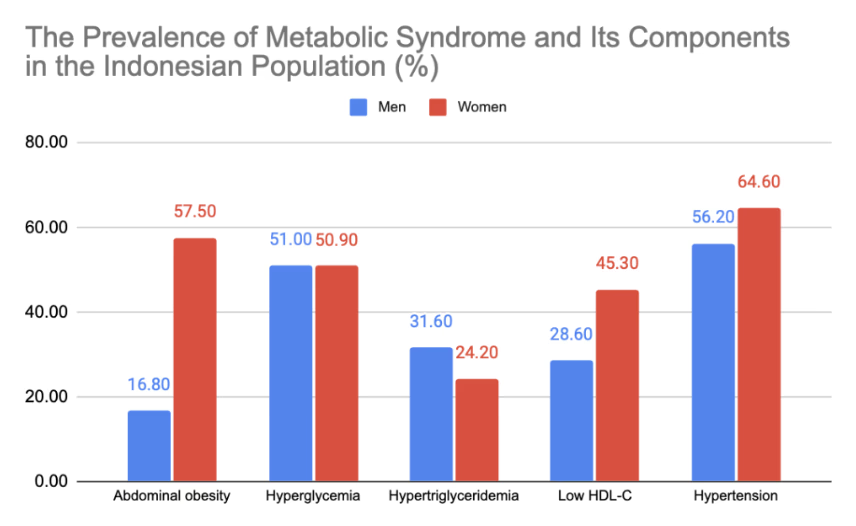
The prevalence of metabolic syndrome was 28% and 46% in Indonesian men and women.
In Indonesia, the prevalence of metabolic syndrome components is as follows:
- Hypertension: 61.0% (the most prominent component)
- Hyperglycemia: 51.0% (second most common component)
- Abdominal Obesity: 41.5%
- Low HDL-C: 38.7%
- Hypertriglyceridemia: 27.1%
Metabolic syndrome, significantly elevates health risks. Patients with this condition are estimated to have a 2-fold increased risk of atherosclerotic cardiovascular diseases and a 5-fold increased risk of developing diabetes mellitus compared to the general population.
Top 10 Causes of Death
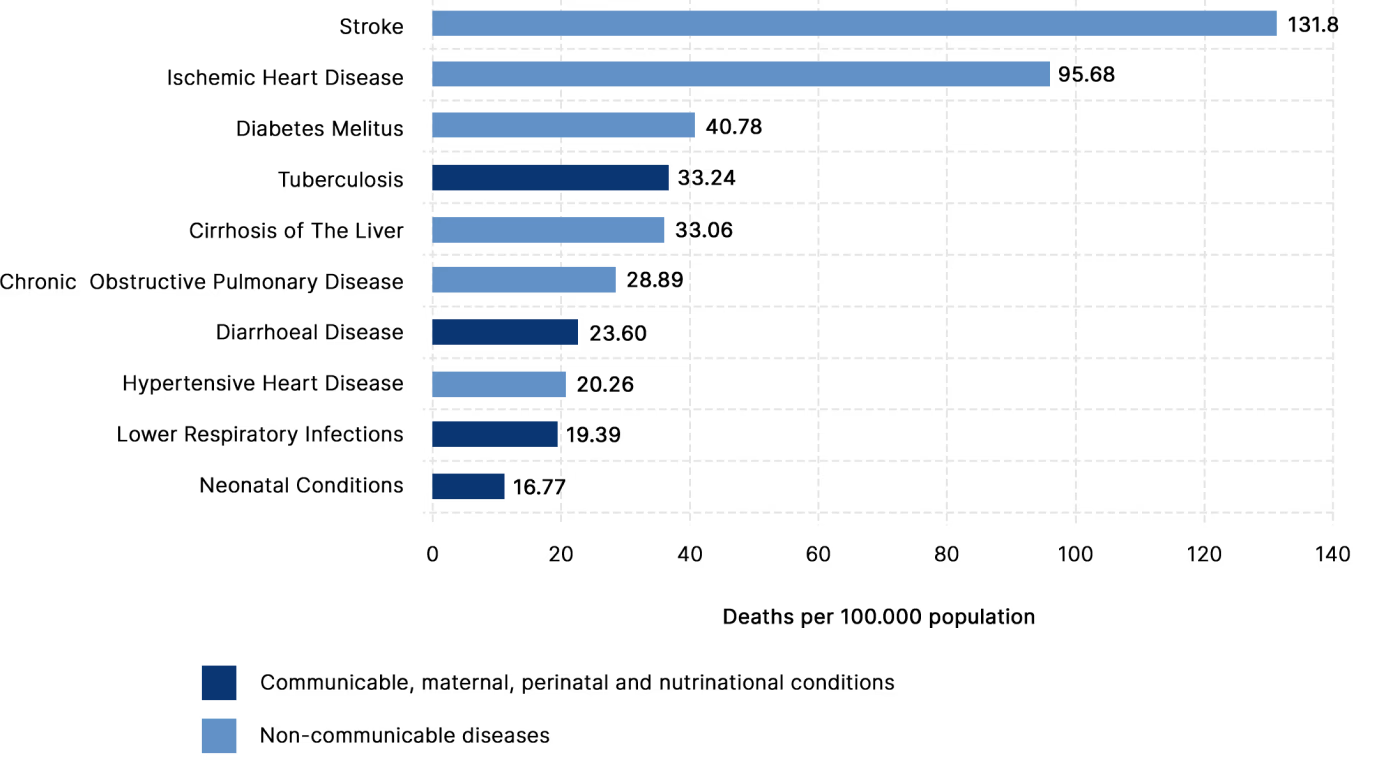
Metabolic syndromes are key contributors to the top three causes of death in Indonesia, with cardiovascular diseases leading the list of non-communicable diseases (NCDs). Stroke and ischemic heart disease, which are heavily influenced by conditions like hypertension, obesity, and diabetes, with 131.8 and 95.68 cases per 100,000 population respectively, rank highest. These metabolic conditions, including diabetes, are the primary drivers behind the nation's most fatal diseases.
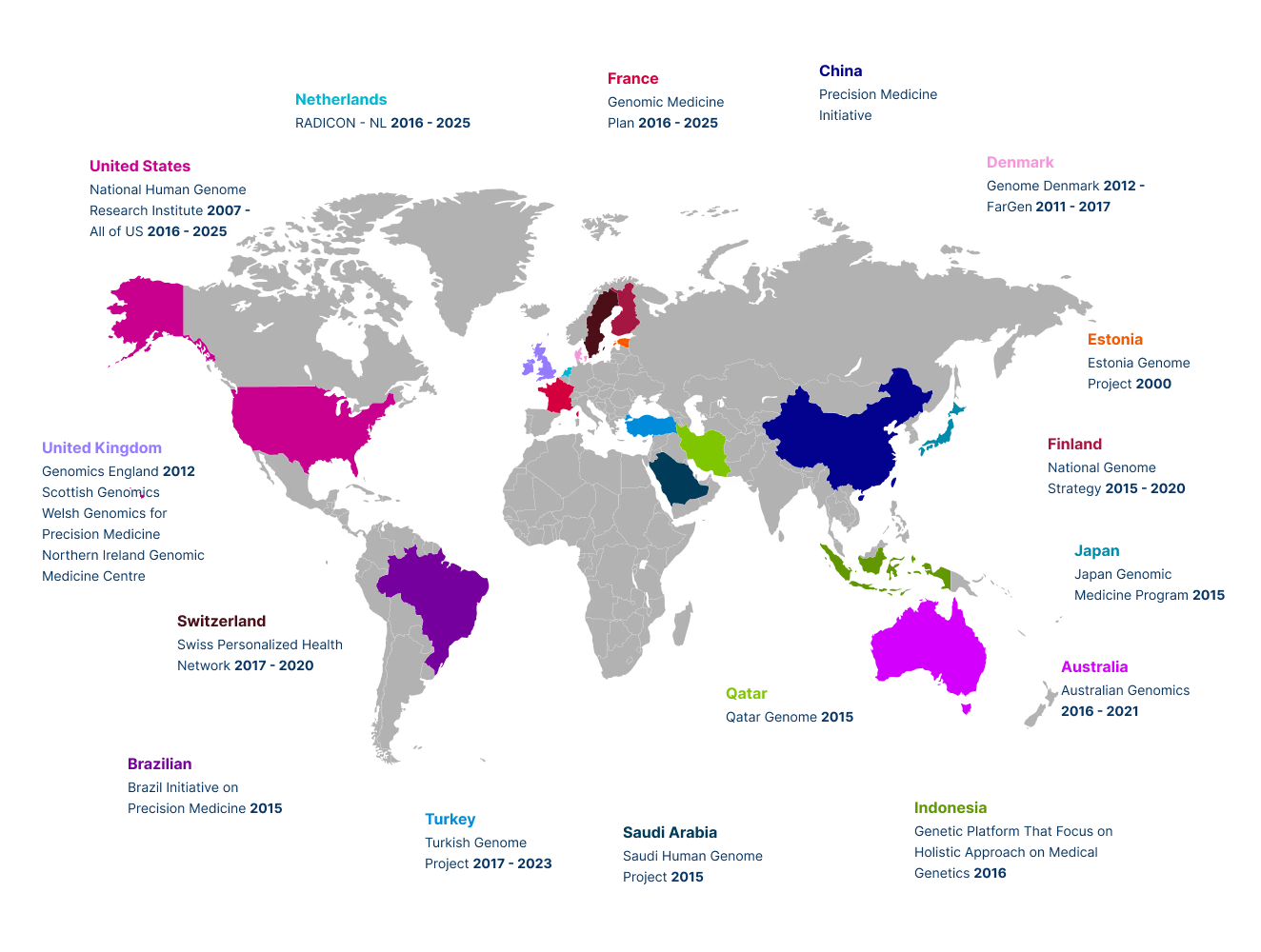
Genomic's Role in Precision Medicine
Genomics is transforming healthcare through personalized medicine. While global initiatives leverage genomics for diseases, Indonesia's genomics adoption, especially for genetic disorders, lags behind.
Metabolic conditions heavily contribute to coronary heart disease (CHD) and stroke, causing 470,000 deaths annually in Indonesia. Cigarette smoking (64.9%) is the most prevalent risk factor among men, followed by elevated total cholesterol (30%), hypertension (22.8%), excess body weight (19.6%), and diabetes (5.6%). On the other hand, in women, elevated total cholesterol (39.6%) is the leading risk factor, followed by excess body weight (32.9%), hypertension (28.8%), and diabetes (7.7%). Metabolic abnormalities significantly contribute to these outcomes, accounting for 78% and 98% of CHD of death in men and women, respectively.
Current strategies for metabolic diseases prevention, early diagnosis, and treatment often fall short due to their generalized approach. Lifestyle modifications, such as diet and exercise, are crucial but do not account for individual genetic differences. Early diagnosis typically relies on routine screenings like cholesterol and blood pressure tests, as well as imaging tests such as echocardiograms and angiograms for cardiovascular diseases. However, these methods can miss early signs in individuals who are genetically predisposed to metabolic diseases. Treatment options, while effective for some, may not work optimally for all due to genetic variations, leading to inconsistent responses and potential side effects, such as adverse reactions to statins or antihypertensive drugs.
Clinico-genomic research offers a solution by integrating genetic data into metabolic diseases. This approach enables personalized prevention strategies, early and precise diagnosis, and tailored treatments based on an individual's unique genetic makeup. By uncovering genetic markers linked to metabolic diseases, researchers can develop more accurate predictive models and innovative therapies. Clinico-genomic research promises to enhance metabolic health outcomes, reduce disease incidence, and pave the way for longer, healthier lives.
Sources :
- Hussain MA, Al Mamun A, Peters SA, Woodward M, Huxley RR. The Burden of Cardiovascular Disease Attributable to Major Modifiable Risk Factors in Indonesia. Journal of Epidemiology. 2016;26(10):515-521. doi:https://doi.org/10.2188/jea.je20150178
- AHA names top advances in cardiovascular disease research for 2023. www.heart.org. Published January 2, 2024.
- Jacobs DR, Woo JG, Sinaiko AR, et al. Childhood Cardiovascular Risk Factors and Adult Cardiovascular Events. New England Journal of Medicine. 2022;386(20). doi:https://doi.org/10.1056/nejmoa2109191
- NCBI - PMC5037248
- NCBI - NBK459248
- NCBI - PMC6947940